Do you have ongoing mouth pain, swelling, bad breath, or trouble swallowing? These could mean you have a mouth infection that needs quick action. Mouth infections can be simple annoyances or serious issues that need emergency care if ignored.
Spotting the early signs is key to getting the right treatment fast. At Istinye Dental Hospital, we focus on you with our care. We use the latest in dentistry to help you get the best oral health.
Mouth infections are a big worry worldwide, affecting millions. About 200,000 Americans go to the emergency room each year for severe dental problems or abscesses.
Key Takeaways
- Spotting early signs of mouth infections is vital for quick treatment.
- Mouth infections can be from mild to very serious.
- Istinye Dental Hospital offers a patient-focused approach with the latest dentistry.
- Every year, about 200,000 Americans visit emergency rooms for severe dental issues.
- Getting dental care on time is key to avoiding bigger problems.
Understanding Mouth Infections: An Overview
It’s important to know about mouth infections to keep your mouth healthy. These infections can happen in different parts of your mouth, like your gums, teeth, and mucous membranes.
Definition and Prevalence of Oral Infections
Mouth infections happen when harmful germs attack your mouth’s tissues. They can show up as gum problems, tooth abscesses, or oral thrush. Many people get mouth infections at some point in their lives.
Key statistics on oral infections include:
- Periodontal disease affects over 47% of adults in the United States.
- Oral candidiasis (thrush) is common among individuals with compromised immune systems.
- Viral infections like herpes simplex can cause recurrent oral lesions.
Impact on Overall Health
Mouth infections can affect more than just your mouth. They can also harm your overall health. Studies link them to heart disease, diabetes, and respiratory infections. This is because the inflammation from these infections can spread.
The consequences of untreated mouth infections can be severe. They can cause pain, swelling, and even spread to other parts of your body. So, it’s key to catch the signs early and see a dentist.
- Bacterial infections, such as periodontitis and tooth abscesses.
- Fungal infections, like oral candidiasis.
- Viral infections, including herpes simplex virus.
Each infection has its own signs and needs the right treatment. Knowing the differences helps in managing and preventing them.
Common Types of Mouth Infections
It’s important to know about the different mouth infections. They can be caused by bacteria, fungi, or viruses. Each one needs a specific treatment.
Bacterial Infections
Bacterial infections in the mouth show symptoms like redness and swelling. You might also have bad breath, pain, and fever. In serious cases, you could feel sick all over.
Examples include gum infections and tooth abscesses. These are serious and need quick attention.
Fungal Infections
Fungal infections, like oral thrush, show up as white patches. They often happen in people with weak immune systems. This includes those on chemotherapy or with diabetes.
Viral Infections
Viral infections can cause painful sores in your mouth. For example, herpes simplex virus (HSV) causes cold sores. Varicella-zoster virus can turn into shingles and affect your mouth too.
Here’s a quick guide to these infections:
| Infection Type | Common Symptoms | Typical Characteristics |
|---|---|---|
| Bacterial | Redness, swelling, pain, halitosis | Gum infection, tooth abscess |
| Fungal | White patches, discomfort | Oral thrush, more common in immunocompromised individuals |
| Viral | Painful sores, lesions | Cold sores (HSV), shingles (varicella-zoster virus) |
Knowing what kind of mouth infection you have is key. It helps you get the right treatment. By understanding the symptoms of bacterial, fungal, and viral infections, you can take care of yourself better.
Symptoms of Mouth Infections: Key Warning Signs
It’s important to know the signs of mouth infections to get treatment early. These infections can be bacterial, fungal, or viral. Each has its own symptoms.
General Symptoms Across All Types
Though each infection is different, some symptoms are common. These include:
- Persistent oral pain or discomfort
- Red or swollen gums and oral tissues
- White patches or lesions in the mouth
- Bad breath or an unpleasant taste
- Difficulty swallowing or speaking
- Swollen lymph nodes in the neck
Dental experts say early detection is key. It can lead to better treatment and stop the infection from spreading.
“The presence of white patches or lesions in the mouth can be a sign of a fungal infection, such as oral thrush. It’s essential to consult a dentist if you notice any unusual changes in your mouth.”
When Symptoms Indicate a Serious Condition
Some symptoms mean you need to see a doctor right away. If not treated, these infections can get worse. They might even spread to other parts of your body.
| Symptom | Possible Indication |
|---|---|
| Severe pain or swelling | Abscess or severe infection |
| Difficulty swallowing or breathing | Spread of infection to the throat or airway |
| Fever or chills | Systemic infection |
Knowing the signs of mouth infections helps keep your mouth healthy. It’s important to act quickly if you see any serious symptoms.
Bacterial Infection Mouth Symptoms in Detail
Knowing the signs of bacterial infections in the mouth is key to treating them well. These infections can show different symptoms, ranging from mild to severe.
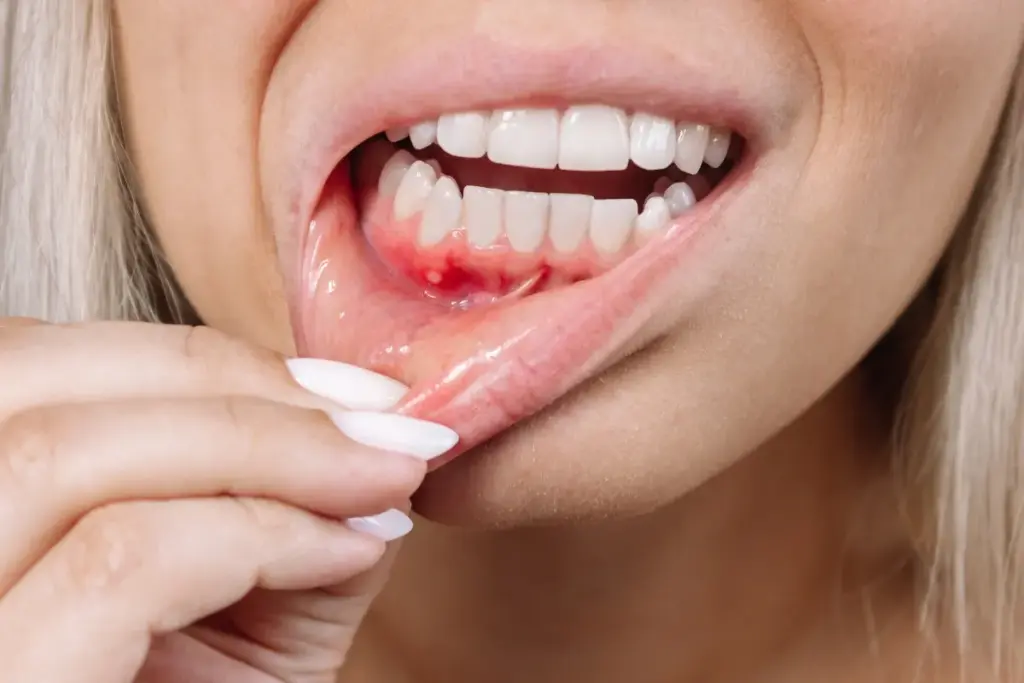
Gum Infection Symptoms
Gum infections, or periodontal diseases, happen when bacteria build up in the gums. Look out for these signs:
- Redness and Swelling: Gums might turn red, swell, and feel tender.
- Bleeding Gums: Gums can bleed when brushing or flossing, even gently.
- Bad Breath: If you have bad breath or a bad taste, it could mean gum infection.
- Pain or Discomfort: Gums might hurt, more so when eating or drinking hot or cold things.
Tooth Abscess Signs
A tooth abscess is a serious issue that needs quick dental help. Watch for these signs:
- Severe Toothache: Pain can be very strong and spread to the jaw, ear, or neck.
- Sensitivity: Teeth might hurt more when exposed to hot or cold, or when pressed.
- Swollen Lymph Nodes: Lymph nodes under the jaw or in the neck might swell.
- Fever: A high fever can happen with a tooth abscess, showing the body’s fight against infection.
Severe Bacterial Infection Indicators
Severe bacterial infections can spread, causing bigger health problems. Look out for these signs:
- Systemic Symptoms: Feeling unwell, fever, or chills can happen as the infection spreads.
- Swelling: Big swelling in the face, cheek, or jaw can mean the infection is spreading.
- Difficulty Swallowing: Swelling can make it hard to swallow or breathe in severe cases.
- Persistent Pain: Pain that keeps getting worse or doesn’t go away, even with home care or over-the-counter treatments.
If you notice any of these symptoms, get dental care right away. This helps prevent bigger problems and ensures the right treatment.
How to Identify Fungal Infections in the Mouth
Fungal infections in the mouth, like oral thrush, show clear signs. They often hit people with weak immune systems. This includes older adults and those on certain meds like antibiotics or steroids.
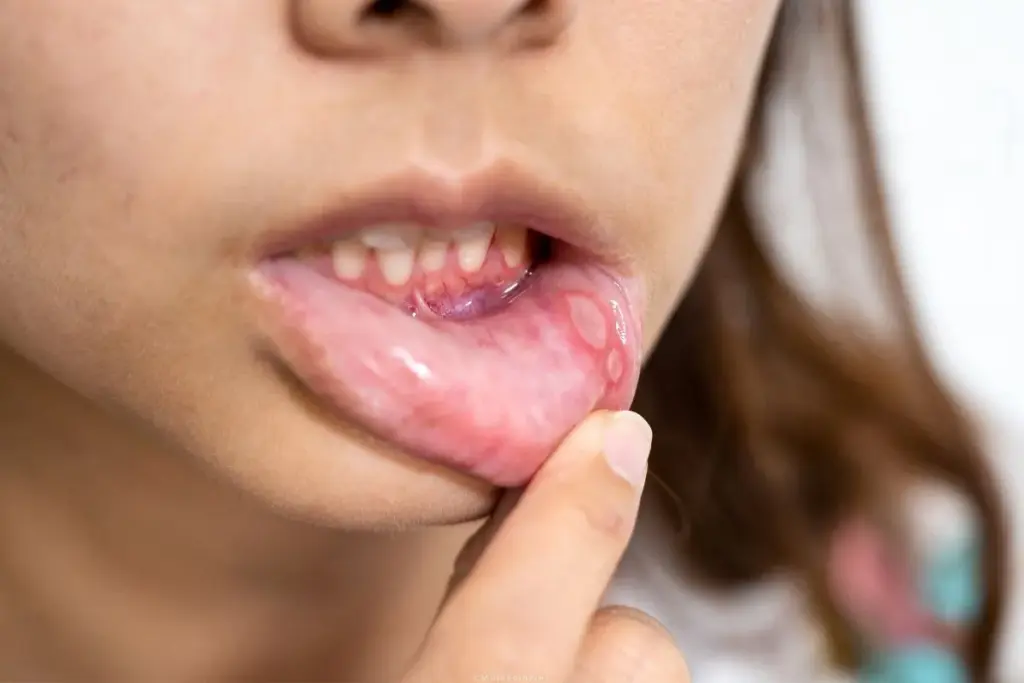
Characteristic White Patches and Lesions
Oral thrush shows up as white patches or lesions. They can be found on the tongue, inner cheeks, and sometimes the roof of the mouth or throat. These patches can be wiped off, revealing red, inflamed areas that may bleed slightly. Seeing these white patches is a big sign of a fungal infection.
Not all lesions are white; they can be red or mixed. It’s important to watch for any mouth changes. If you see something odd, talk to a healthcare pro.
Associated Discomfort and Pain Patterns
Fungal infections can make your mouth hurt, feel sore, or burn. This pain is worse when eating or swallowing. Some people get cracking at the mouth corners, called angular cheilitis, which hurts and might be fungal.
The pain from these infections can be mild or very bad. Severe cases can make it hard to eat or swallow. This can lead to not getting enough nutrients or dehydration, which is risky for the elderly.
Key symptoms to watch for include:
- White patches or lesions on the tongue, inner cheeks, or throat
- Redness or inflammation under the white patches
- Pain or discomfort when eating or swallowing
- Cracking at the corners of the mouth
If you notice these symptoms, see a healthcare pro right away. They can give you a proper diagnosis and treatment. Catching and treating fungal infections early helps keep your mouth healthy.
Recognizing Viral Mouth Infections
It’s important to know the signs of viral mouth infections to keep your mouth healthy. These infections can cause mild discomfort or severe pain. They can be triggered by stress, hormonal changes, or certain medicines.
Distinctive Sores and Blisters
Viral mouth infections often show up as sores and blisters. Cold sores are a common example. They are caused by the herpes simplex virus. These sores look like small blisters on the lips, tongue, or gums.
- Painful blisters or sores in the mouth or on the lips
- Redness and swelling around the affected area
- Itching or burning sensation before the sore appears
Accompanying Systemic Symptoms
Viral mouth infections can also have symptoms that affect your whole body. These might include:
- Fever or swollen lymph nodes
- Feeling unwell or tired
- Headaches or sore throat
Spotting these symptoms can help you get the right treatment. If you keep getting these symptoms, see a doctor for help.
How to Tell If You Have a Mouth Infection: Self-Assessment Guide
Knowing the signs of mouth infections is key for early treatment. Regular dental visits and good oral care can lower the risk. Spotting early signs can help you act fast.
Visual Inspection Techniques
Looking at your mouth can help spot infections. Look for redness, swelling, or white patches on your gums, tongue, or cheeks.
Use a mirror to check all parts of your mouth. Look for any unusual changes, like:
- Unusual redness or swelling
- White or yellow patches
- Sores or ulcers
- Bleeding gums
Symptom Tracking and Documentation
Tracking your symptoms can help find patterns. Keep a log of any mouth issues, like:
| Symptom | Date | Severity |
|---|---|---|
| Gum pain | 02/10 | Mild |
| White patches | 02/12 | Moderate |
| Bleeding gums | 02/15 | Severe |
Recording your symptoms helps your dentist diagnose and treat better.
Early detection is key to managing mouth infections. Visual checks and tracking symptoms are good steps for your oral health.
Professional Diagnosis of Oral Infections
A dental professional’s diagnosis is key to understanding an oral infection. They create a treatment plan based on it. When you see a dentist with mouth infection symptoms, they will examine you thoroughly.
Dental Examination Process
The dentist will look at your mouth for signs of infection. They check for redness, swelling, and pus. They also feel your gums and teeth for tenderness.
Key components of the examination include:
- Visual inspection of the mouth
- Palpation to check for tenderness
- Assessment of gum and tooth health
Diagnostic Tests and Procedures
The dentist might use X-rays or swabs for lab tests. These help find out what kind of infection you have and how bad it is.
Common diagnostic tests include:
- X-rays to assess bone loss or abscesses
- Swabs for culture and sensitivity testing
- Blood tests to check for underlying conditions
Differential Diagnosis Considerations
Dentists also rule out other conditions that might look like a mouth infection. They look at your medical history, symptoms, and test results. This helps them make an accurate diagnosis.
Factors considered in differential diagnosis include:
- Medical history and current health status
- Symptom severity and duration
- Results from diagnostic tests
Dental professionals use a detailed examination, tests, and differential diagnosis. This way, they can give you a correct diagnosis and a good treatment plan for mouth infections.
Risk Factors That Increase Susceptibility to Mouth Infections
Some medical conditions and lifestyle choices can make you more likely to get mouth infections. Knowing these risk factors is key to preventing and treating them early.
Medical Conditions and Compromised Immunity
People with certain health issues are more at risk for mouth infections. For example, diabetes can weaken the body’s defense against infections. Those with compromised immune systems, like those on chemotherapy or with HIV/AIDS, are also more likely to get oral infections.
- Autoimmune diseases like Sjögren’s syndrome can raise the risk by making it hard for the mouth to make saliva. Saliva is important for keeping the mouth healthy.
- Cancer treatments that weaken the immune system can also make patients more prone to mouth infections.
Dental experts say, “Patients with weakened immunity need extra care to prevent and manage mouth infections well.”
Lifestyle and Oral Hygiene Factors
How you live and take care of your mouth can also affect your risk of getting mouth infections. Poor oral hygiene lets bacteria and fungi build up in your mouth.
- Smoking and using tobacco products can raise the risk of mouth infections. They weaken the body’s defense and harm oral tissues directly.
- Diet matters too. Eating a lot of sugars and acids can lead to tooth decay and other issues that may cause infections.
Good oral hygiene, like brushing and flossing regularly, and avoiding harmful lifestyle choices can lower your risk of mouth infections.
Treatment Approaches for Different Mouth Infections
Treating mouth infections involves various methods, from prescription drugs to home care. The type and severity of the infection determine the best treatment.
Prescription Medications and Professional Treatments
For bacterial infections, antibiotics are often used to kill the bacteria. Severe gum infections or tooth abscesses may need dental cleaning or surgery. Fungal infections, like oral thrush, are treated with antifungal medications, available as mouthwashes or lozenges.
Viral infections, such as herpes simplex virus, may need antiviral medications to control symptoms. Sometimes, laser therapy or other advanced treatments are suggested to aid healing and ease pain.
| Infection Type | Common Treatments |
|---|---|
| Bacterial | Antibiotics, Professional Dental Cleaning |
| Fungal | Antifungal Medications |
| Viral | Antiviral Medications, Laser Therapy |
Home Care and Over-the-Counter Options
Home care is also important for managing mouth infections. Good oral hygiene is key, including brushing and flossing regularly. Antiseptic mouthwashes can help reduce bacteria.
For pain relief, over-the-counter pain relievers and topical anesthetics can help. Always follow your dentist’s advice for safe and effective treatment.
“Maintaining good oral hygiene is key in preventing and managing mouth infections. Regular dental check-ups can catch issues early, leading to timely treatment.”
Prevention Strategies for Maintaining Oral Health
Keeping our mouths healthy is key to our overall well-being. Prevention is the best way to fight off mouth infections and keep our smiles bright.
Daily Oral Hygiene Best Practices
Good oral hygiene is the base of a healthy mouth. It means doing a few simple things every day:
- Brushing teeth at least twice a day with fluoride toothpaste to remove plaque and bacteria.
- Flossing daily to clean between teeth where a toothbrush cannot reach.
- Rinsing with an antibacterial mouthwash to kill bacteria and freshen breath.
Proper brushing technique is very important. Use a soft-bristled toothbrush and brush in circular motions. Make sure to clean all tooth surfaces. Change your toothbrush every three to four months or sooner if it gets frayed.
Regular Professional Care and Check-ups
While daily care is vital, regular dental check-ups are also key. These visits help catch problems early and prevent bigger issues.
At a dental check-up, your dentist will:
- Examine your mouth, teeth, and gums thoroughly.
- Remove plaque and tartar through professional cleaning.
- Look for signs of gum disease or tooth decay.
- Give you advice on how to keep your mouth healthy.
Going for regular check-ups is a smart move for your mouth. It helps avoid expensive and painful dental problems later on.
Conclusion: Taking Action Against Mouth Infections
Knowing the signs and dangers of mouth infections is key to keeping your mouth healthy. Spotting the warning signs early and acting fast can stop problems from getting worse. This ensures you get the right treatment on time.
Preventing mouth infections means keeping up with good oral care. Brush and floss regularly and see a dentist when you need to. Catching and treating infections early can make a big difference and lower the chance of serious issues.
By focusing on your oral health and staying ahead, you can avoid the dangers of mouth infections. Regular dental visits and good oral hygiene habits are vital. They help keep your smile bright and your overall health strong.
FAQ
What are the common symptoms of a mouth infection?
Symptoms include pain, swelling, and redness. You might also see pus. Bad breath, fever, and swollen lymph nodes are other signs.
How do I know if I have a bacterial infection in my mouth?
Look for gum infection signs like redness and swelling. Tooth abscesses show as severe pain and pus.
What are the signs of a fungal infection in the mouth?
Fungal infections show as white patches and lesions. You might feel discomfort and pain.
How can I identify a viral mouth infection?
Viral infections have distinctive sores and blisters. They often come with fever and fatigue.
What should I look for during a self-assessment for mouth infections?
Look for redness, swelling, and white patches. Also, track pain and discomfort.
What can I expect during a professional diagnosis of an oral infection?
A dental exam includes a visual check and tests like X-rays. Your medical history is also reviewed.
What are the risk factors for developing a mouth infection?
Risk factors include diabetes and smoking. Poor oral hygiene is also a risk.
How are mouth infections typically treated?
Treatment depends on the infection type. It may include medications or professional treatments. Home care like saltwater rinses is also used.
How can I prevent mouth infections?
Prevent them with good oral hygiene. Brush and floss daily. Regular dental check-ups are key.
What are the consequences of leaving a mouth infection untreated?
Untreated infections can cause abscesses and bone loss. They can even lead to systemic infections.
Can mouth infections be a sign of an underlying health issue?
Yes, they can signal a health problem. This includes a weak immune system or diabetes.
National Center for Biotechnology Information. Evidence-Based Medical Guidance. Retrieved from https://www.ncbi.nlm.nih.gov/books/NBK542165/
